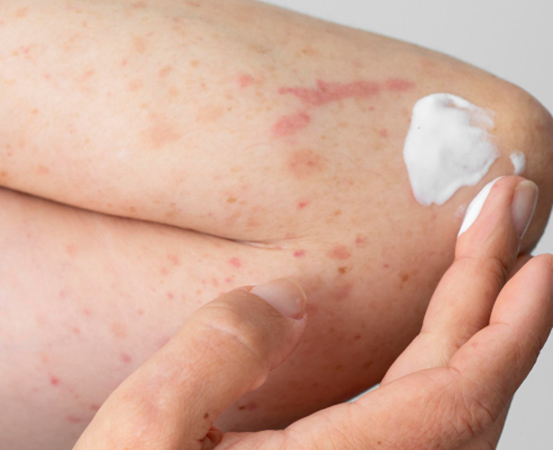
For Neeta Ashok, a 36-year-old working woman from Bengaluru, urticaria hit when she was enjoying the arrival of her newborn baby five years ago. The unexplained itching and rashes on her hands, elbows, thighs and palms would subside through medicines, but would keep reappearing.
“I still remember how the etching began on the hands and palms suddenly in early 2017, and it continued to be a nightmare after that too. I could see large red spots on the hands, elbows, thighs and palms. I first thought I had touched some plant or ate something that may have turned out to be allergic. The doctors diagnosed it as urticaria,” says Neeta.
Also called hives, urticaria is a skin allergy characterised by symptoms such as itchy, raised, red or skin-coloured welts, says Dr Smriti Naswa Singh, consultant dermatologist and cosmetic dermatologist, Fortis Hospital, Mumbai. “It is said. ‘Anything under the sun, including the sun, can cause allergies.’”
According to Dr Sravya C Tipirneni, consultant dermatologist and cosmetologist at Manipal Hospitals, Bengaluru, one in five people will have at least one or two episodes of urticaria at any point of time in life.
Common causes and types
Dr Singh lists out a few causes and types of hives:
- hereditary — called atopic urticaria, where some or other allergic manifestation is present in a family (like bronchial asthma, allergic rhinitis, allergic conjunctivitis, allergic eczema or atopic dermatitis)
- drugs/medicines, common painkillers, antibiotics such as the penicillin group, some anaesthetics and vaccines
- foods (high in protein) like seafood, cow milk, egg and nuts
- fragrance agents, dust, environmental allergens like pollens, parthenium/wild grass, sun
- aquagenic urticaria — caused by water (patients get hives after a bath)
- cholinergic urticaria — caused by a temperature change and sudden exposure to hot or cold air
- pressure urticaria — caused by the pressure of the shoulder strap of a bag or wristwatch (thereby causing localised urticaria)
- emotional urticaria — caused by mental stress
Dr Singh says the lifetime prevalence of urticaria is up to 22 per cent and point prevalence (at any given point of time) is one per cent. She says chronic urticaria can commonly be either atopic (hereditary) or autoimmune (where other autoimmune conditions like autoimmune hypothyroidism may coexist).
Triggers
Dr Tipirneni says the most common triggers are either food items or external contact with some kind of allergic substance or pollen or dust in the environment.
Dr Singh lists some common triggers to be avoided by people who are prone to urticaria:
- sudden changes of temperature (like being in the hot sun and going immediately to an AC room)
- using medicines without a prescription from doctors
- if one has known allergy, they should abstain from exposing themselves to it
- sweating
- perfume and colouring agents in cosmetic products
- colouring agents in foods
- cow milk, eggs and animal proteins in children below the age of one. As these proteins are the most typical causes of allergies in infants, they can manifest as urticaria or gut issues or atopic dermatitis (acute dry skin)
However, the causes cannot be pinpointed as being caused by a specific allergen each time. In Neeta’s case too, the cause was not found. “I used to be preoccupied with the fear of red patches and itching all the time. It affected my everyday work in office. I always carried my medicines with me,” she tells Happiest Health.
While no allergen was found in her case, it was said to be chronic idiopathic urticaria. “Urticaria is not contagious. If I get hives, the person next to me does not get it. However, there is lack of awareness and I did face stigma when the red spots on my hands and palms were visible,” Neeta says.
Dr Singh says urticaria is diagnosable, and a dermatologist can help treat the disease. It looks like mosquito bites and is very itchy, and typically the lesions subside within 24 hours — only to come back again.
There is no test that can detect urticaria, says Dr Tipirneni. “A general blood test that can show high eosinophil count or a high IgE count may help in diagnosing it,” she says. Asthmatic people are more prone to this, she says.
Link to childhood asthma
Recalling a recent case, Dr Singh says the patient had asthma in childhood but it healed as he entered his teenage years. “In his mid-thirties, the patient started to have hives,” she says. “The hives would subside with a course of antihistamines, only to recur after 24 hours. Slowly the hives became chronic, and they used to reduce with the antihistamines, but the recurrences would always be there. With the detailed follow-up and history-taking, two things — food and emotional stress — came out as significantly causing the exacerbation of the hives,” she said.
For some people, wheat or all-purpose flour can turn out to be an allergen.
“In some cases, hives appear whenever the affected person takes wheat,” says Dr Singh. “This is due to poor gut health. When a person has allergic manifestations, the gut health is poor, and while trying to improve the symptoms, gut health recovery is of utmost importance. Gut bacteria are the soldiers of the gut that feed on fibre. Wheat flour and other refined and processed foods lack fibre, and in a poor gut patient, the consumption of such foods would immediately manifest allergic rashes.”
Emotional stress as trigger
Dr Singh says the root cause of hives, which also lead to decreasing gut health, is emotional stress due to professional pressure. “Ninety per cent of the neurotransmitters in the body are secreted in the gut, so a strong gut also leads to a happier and calmer person,” she says. “The poor gut — or ‘leaky gut’ with a lack of lining of good gut bacteria — not only manifests allergies but the symptoms are also manifested in the presence of mental stress, whether personal or professional.
“In this patient [whose hobby was painting], interestingly, devoting one hour to painting daily improved urticaria — to the [extent] that on the days the patient would paint, hives wouldn’t appear. On the days when the patient was stressed, the hives would start appearing again.”
Treatment of Urticaria
Dermatologists say the typical symptoms of urticaria must not be ignored and seeking medical advice is essential to reduce its severity. Those dealing with urticaria should remain on medication until the hives stop reoccurring.
“Within six months, it turned out to be chronic urticaria,” says Neeta. “I had reached a stage where the dosage had to be increased and I had to take medicines after every 12 hours. It used to be the worst during the winter months. Once it began, it used to continue for over three to four months. I was also on immunoglobulin injections, but that did not yield much result in my case.”
Neeta says a dermatologist put her on B12 supplements along with antihistamines, and she has had no rashes or itching since 2020.
Talking about the treatment aspects in detail, Dr Singh says:
- [It is important to] find the aggravating or causation factors for the condition and help the patient to avoid them. This can be found after a detailed history discussion of the patient with the doctor
- Antihistamines are the mainstay of treatment for urticaria. Second-generation antihistamines are also preferred
- If urticaria is severe, oral steroids are added for a short time
- The line of treatment for adults and children is similar
- In the case of angioedema (swelling under the skin), intravenous steroids and antihistamines are suggested in an emergency or hospital set-up


















2 Responses
Interesting read.
Thanks for the positive response!