
As we navigated the uncharted territory of the pandemic, our attention was fixated on keeping our lungs healthy. From wearing masks to filter out particulates and viruses, to giving up smoking, we did a lot to promote lung health. But we may not have considered a major aspect of helping us breathe better – our guts.
New research suggests that our gut health may play a crucial role in the functioning of our respiratory system. Enter the gut-lung axis – a fascinating relationship that has piqued the interest of scientists and health enthusiasts alike. By exploring the intricate connection between these two organs, we look to find ways to leverage it to optimize our overall health.
From reducing the risk of respiratory infections to improving lung function, the gut-lung axis is an area of research that holds promise for the treatment of a variety of health conditions.
The science behind the gut-lung connection
“The microbiome has been subject to many studies in connection to lung diseases,” Dr Kamal Dua, senior lecturer at University of Technology, Sydney, says in an online interaction with Happiest Health. His research studies the gut-lung axis in lung conditions such as chronic obstructive pulmonary disorder (COPD), asthma and lung cancer. Additionally, he also works on making novel medication-delivery systems for chronic airway diseases that could be translated into a clinical setting one day.
“When we look at lung diseases, we look at pathogenesis – basically the influx of some molecules in a particular body part, which triggers a lot of inflammation,” he says.
Taking asthma as an example, Dr Dua says inhaling a lot of smoke or allergens triggers your epithelial cells (the cell victims in lung diseases) that lead to alternations in their morphology. This causes excretion of mucus and collagen into the airways.
“Once there is accumulation of mucus, you have difficulty in breathing. This is because cells are triggering the inflammatory pathways to release molecules such as cytokines,” he adds.
It essentially means when inflammatory markers rise in any condition, it leads to the development of the condition.
“There is so much of microflora in your gut that can help in reactivating or reversing those inflammatory cytokines to the normal levels. It means indirectly, those microbiomes can help the lungs through the gut by producing some beneficial effects. This is what is called as the gut-lung axis,” explains Dua.
Balancing the gut with a dose of good bacteria
The question now arises on how to use what we know about the gut-lung axis to design better therapeutics, perhaps one that looks at modifying the gut microbiome.
C Vivek Lal, founder and CEO of Alveolus and ResBiotic and the director of the Pulmonary Microbiome Lab at the University of Alabama at Birmingham, has been applying microbiome science to design a probiotic that acts along the gut-lung axis.
In his years as a physician and treating infants with respiratory conditions, Lal realised that the microbes in the gut far outnumber the cells in the body. Using this knowledge, he set out to understand how the gut could possibly be affecting lung disorders.
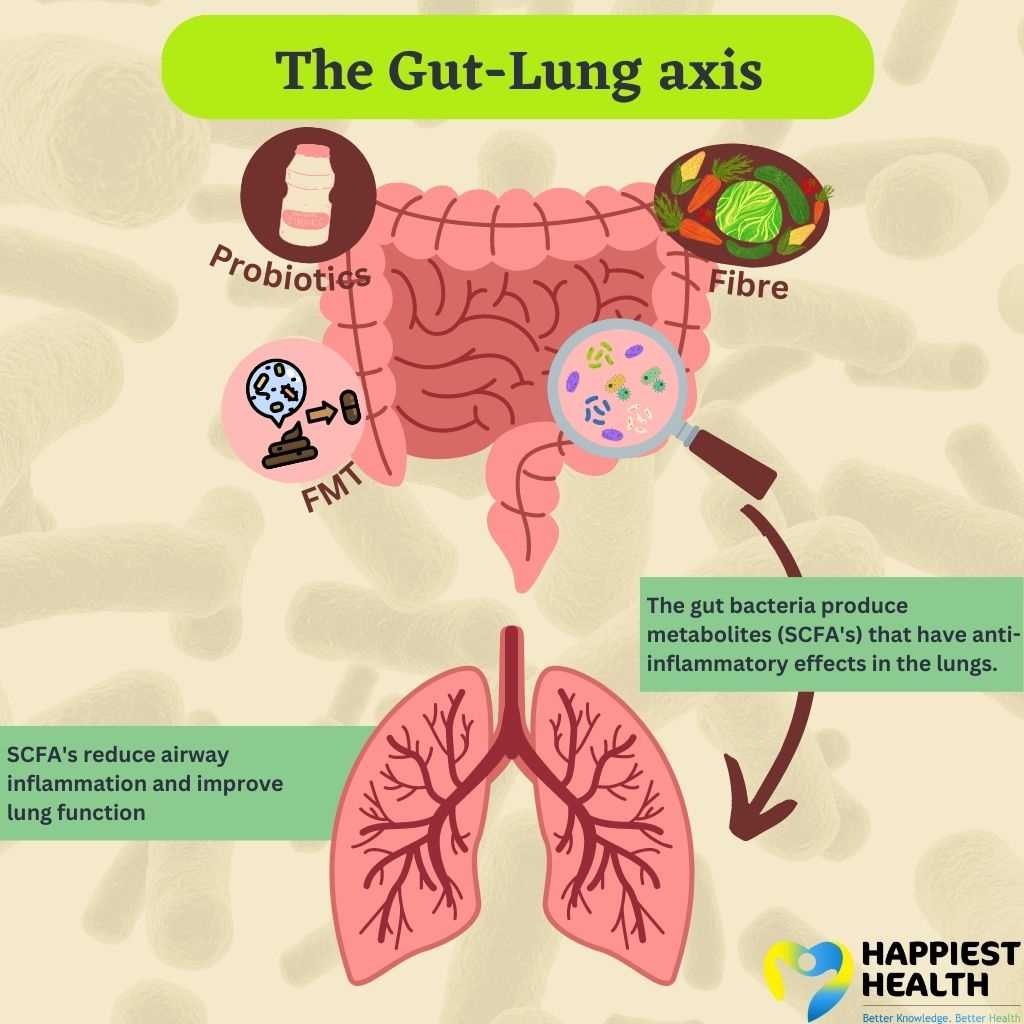
“Some of our first findings was that there were species of bacteria in the gut that were regulating metabolites in the form of short chain fatty acids (SCFAs) that were seen to reduce inflammation in the lungs,” says Lal.
SCFAs are by products made by gut bacteria by the breakdown of nutrients in the gut and are known to play a role in health and disease.
“In this day and age, especially with the western diet, food has become devoid of fibre. The modern way of life is changing the microbiome in the gut drastically. Increasingly, we are seeing people also live in more polluted cities which is leading to a worsening of lung health”, says Lal.
However, we can take steps for better lung functions. One such step is the use of probiotics.
ResBiotics have conducted clinical trials to test the oral administration of a probiotic on lung health. People with asthma were shown to have significant improvements in lung function, along with a more diverse microbial community in the gut.
Nourishing your lungs: how diet influences lung health
What we eat has a profound effect on lung health. The three most important metabolites that regulate the gut-lung axis and manage the immune system are the SCFAs – propionate, butyrate, and acetate, adds Dua.
“Good gut health improves lung function, with the help of intake of nitrites, antioxidants, fibre, and probiotics,” says Dr Priyanka Rohatgi, chief nutritionist, Apollo Hospitals.
“Reactive molecules released on account of metabolism and oxidation can lead to inflammation so eating balanced nutrients as per the requirements helps fight it naturally,” adds Dr Rohatgi.
She mentions that lung health can be improved by:
- Higher intake of antioxidants (found in fruit and vegetables)
- Healthy fats in the form of nuts
- Magnesium
- Reducing salt intake
- Maintaining a normal body mass index
Expanding knowledge on the gut-lung axis
While we still cannot attribute a single microbiome that can improve lung health quickly, research shows that there is a link between microbial influences of immunity and respiratory conditions.
“People are still exploring the gut-lung axis on a cellular and molecular level. They have gone to the level of finding out which pathways are working and getting triggered through this axis” says Dua.
Dr Lal also agrees that the field is evolving and more needs to be learnt of how the microbiome differs depending on population and geographical locations. “Once there is a more thorough understanding, we can look into a more personalised approach to treating a person’s microbiome” he adds.


















3 Responses
Gut health is beautifully explained. I practice the first 4 suggestions but do not know what to do concerning the remaining two. I have asthma and know that constipation causes inflammation in my breathing system
Interesting. New-found knowledge. Definitely the five advice given for good gut health also helps to maintain overall good health. Thanks for the article ??????
Really good infographic!