Just as a baby is tricked into gulping cough syrup, in a study published in Science Immunology on 17 March, researchers have found that the immune system tricks the nervous system into lowering blood pressure and body temperature in response to anaphylaxis.
The study is one of the first to find a functional link between two primal defence mechanisms of the body- thermoregulation and the immune system. The team tracked the series of molecular events from when the allergen entered the bloodstream to triggering the immune reactions of hypothermia and hypotension.
“Our study has revealed that the life-threatening symptoms of anaphylactic shock experienced by allergic individuals are caused, in part, by the organised network of nerve tissue in the body, including the brain and nerves found in the peripheral tissues and organs,” Dr Soman Abraham, senior author and professor at Duke University School of Medicine told Happiest Health.
Anaphylaxis is a severe allergic reaction triggered by the immune system when the body encounters an allergen (an allergy-triggering element). Rashes (hives), itchiness, breathlessness (hypoxia) and a drop in blood pressure (hypotension) and body temperature (hypothermia) are the common symptoms.
Read more: Anaphylaxis: the heart of the matter
The sensory touch
In their experiments in mice, the researchers observed that when the animals had an allergic reaction, they mimicked the body postures they took when exposed to high heat. The team hypothesised that the temperature-controlling neural circuit could be involved in response to allergies.
Dr Abraham said they found how specific immune cells — IgE-mast cells — influenced the brain’s temperature centre, causing hypothermia and hypotension. “This new knowledge suggests that a potential new strategy to prevent anaphylaxis reactions is by targeting these new players,” he said.
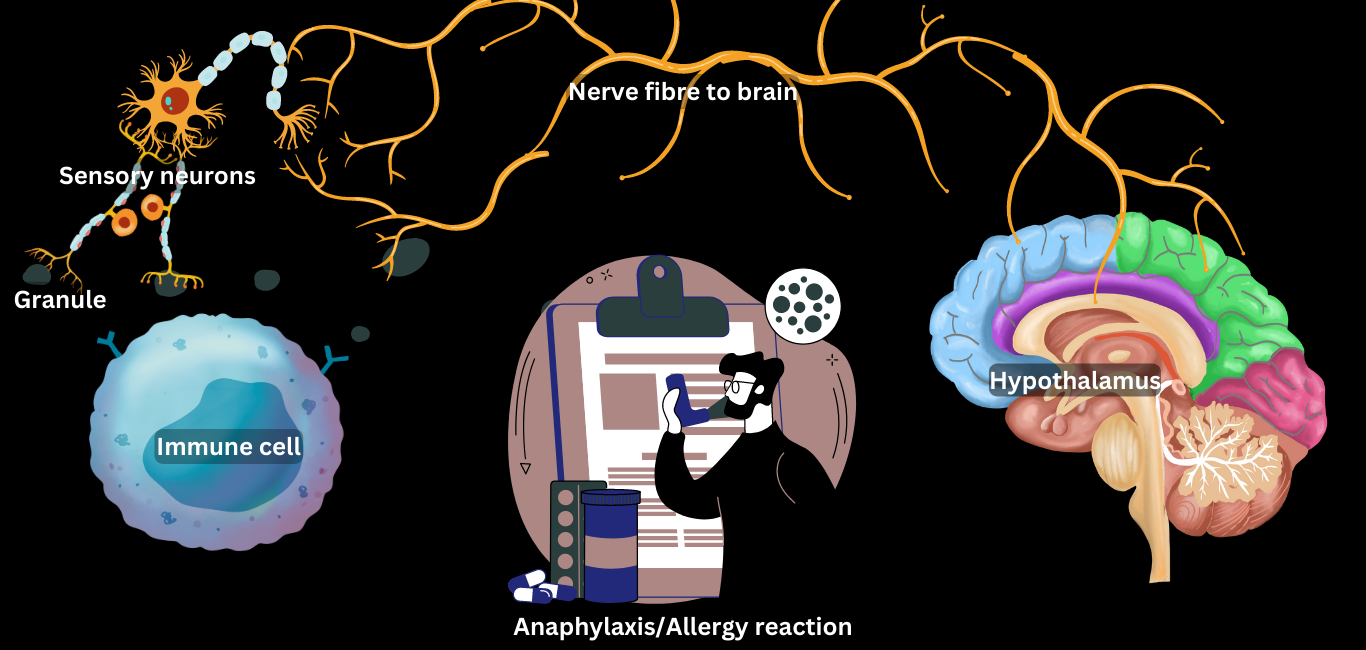
They found the immune IgE-mast cells lingered around the blood vessels, and when an allergen entered the blood, they bound to them. In addition, the mast cells release tiny granules that contain chemicals like histamine, serotonin and enzymes like chymase. Chymase activates the heat-sensitive sensory neurons (TRPV1 neurons) when these granules come in contact with nerve endings.
This tricky activation sends what the researchers call an ‘anaphylaxis-pseudo-heat signal’ to the brain to decrease body temperature – causing hypothermia, which causes a sudden drop in blood pressure.
“The sensory nerves involved in thermal regulation — especially the nerves that sense high environmental temperatures — send the brain a false signal during anaphylaxis that the body is exposed to high temperatures even though it is not the case,” Dr Abraham stated in a statement. He added that this causes a rapid drop in body temperature and blood pressure.
The team conducted further experiments in mice to validate their finding. When the mice were deprived of the chymase enzyme in the blood, there were no symptoms of hypothermia. And when they directly activated the heat sensing TRPV1 neurons, it induced hypothermia and hypotension, as seen in an allergy reaction.
Read more: Hypothalamus: the brain’s smart coordinating centre
Beyond treating symptoms
One of the main reasons why blood pressure drops in an allergic reaction is because the blood vessels dilate. Generally, a shot of epinephrine (EpiPen) constricts the blood vessels to restore normalcy. However, Dr Abraham said this only treats the symptom, not the cause. Whereas their study focuses on the reaction initiated by the nervous system, he said.
“By demonstrating that the nervous system is a key player — not just the immune cells — we now have potential targets for prevention or therapy [of anaphylaxis],” said Chunjing “Evangeline” Bao, the first author of the paper, in the statement. She added that their finding could also be important for conditions like septic shock.