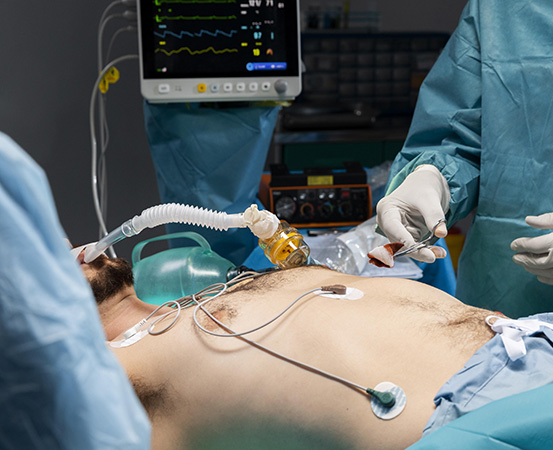
A 63-year-old woman from Nellore, Andhra Pradesh, who suffered from chronic obstructive pulmonary disease (COPD), a chronic lung disease, was admitted to the emergency room of a hospital with severe respiratory distress. Diagnosed with COPD exacerbation with community acquired pneumonia (a type of lung infection acquired outside of a hospital), she was then put on mechanical invasive ventilator for emergency support.
“She was in the intensive care unit (ICU) for two days, where her condition improved with lung-protective ventilation, steroids, antibiotics and other supportive measures,” says Dr Bharath Reddy, a member of the Association of Emergency Physicians of India. Ventilation is the flow of air in and out of the lungs. Invasive mechanical ventilation is administered when the body fails to ventilate itself.
On the second day, the woman was taken off ventilator support; on the third, she walked out of the hospital in a stable condition.
READ MORE :
Warm and humidified air – the magic of nasal cannula
Chest drain: letting your lungs breathe
Respiratory emergency support
“Invasive mechanical ventilation is respiratory support for people whose lungs are failing,” Dr Viny Kantroo, a pulmonologist at Apollo Hospitals, Delhi, says on a call with Happiest Health. “It is given by placing the patient on a machine called a ventilator which oxygenates the body by supplying air directly to the lungs. The decision taken to mechanically ventilate someone depends on their ability to effectively oxygenate themselves.”
According to the US government’s National Library of Medicine, invasive mechanical ventilation is a powerful therapeutic and diagnostic technique in critically ill patients. It differs from non-invasive ventilation in terms of channel of delivery of air to the lungs. In case of invasive ventilation, an endotracheal tube or ETT is used which goes through the windpipe, whereas in non-invasive ventilation, a face mask is used to help a person breathe without invading the body.
“There are certain tubings that connect the ventilator to a person,” says Dr Kantroo, a pulmonologist. “The endotracheal tube is connected to the machine and goes into the windpipe. A positive pressure is developed in the chest which makes sure exchange of gases in the lungs takes place normally and thus oxygenation is assured.”
When is invasive ventilator required?
According to Dr Vivek Padegal, a pulmonologist at Fortis Hospitals, Bengaluru, invasive ventilation is broadly required when someone is not able to breathe due to following reasons:
- Low oxygen levels
- Fast breathing when respiratory muscles tire out
- Not breathing at all because of an underlying issue
- When non-invasive ventilation has failed to improve oxygenation.
“A ventilator is used for buying time for people who are not able to breathe until the underlying issue is fixed,” says Dr Padegal.
According to Dr Kantroo, the primary condition which has caused the lungs to fail should be considered before making the decision of giving invasive ventilation. She says giving invasive ventilation is an important clinical decision wherein many factors are considered, including:
- Brain conditions where consciousness level is affected
- During general anaesthesia as it can inhibit ventilation
- Hemodynamic instability: when someone is on blood pressure-increasing medications.
Complications of invasive mechanical ventilation
The US government’s National Library of Medicine lists a few complications of mechanical ventilation:
- Barotrauma: pressurised air that is pushed into the lungs which can lead to damage due to sudden pressure change in the lungs
- Acute respiratory distress syndrome or ARDS
- Pneumothorax
- Atelectasis: lung damage due to alveolar damage
- Post-extubation stridor: an inspiratory noise which happens when the endotracheal tube is ‘liberated’ or ‘extubated’ from the person. It is a result of laryngeal edema, which is the inflammation of the mucosa of the larynx.
Dr Padegal talks about possible complications:
- Ventilator-acquired pneumonia: lung infection that occurs in a person on a ventilator due to germs entering the lungs through the endotracheal tube. Since the tube goes directly into the mouth, it can cause infections.
- If the patient is not well sedated, the endotracheal tube might be displaced, and the person can get sicker.
- Hemodynamic compromise: happens especially with COPD patients. The air pressure in the lungs can build up, impeding the return of blood to the heart and causes the heart to pump less effectively. This can lead to a drop in the blood pressure. The same can happen if the patient is not sedated well.
“Earlier, issues like barotrauma and volutrauma (excessive stretching of alveoli causing alveolar damage) existed because of large volume of air supplied for every breath taken,” he says. “When the lungs are stiff from an underlying disease, they can develop an air leak, which can cause collapse of the lungs called pneumothorax. But the volume of air was reduced, and such issues were significantly decreased. So, with new practices, complications arise much less as before.”
Dr Kantroo, too, says everything in medical science involves complications. “Doctors weigh the conditions and see how much of risks and benefits are involved in a certain procedure,” she says. “When we consider providing invasive ventilation, it is because the benefits outweigh such known, transient complications like barotrauma and volutrauma.”
Benefits of invasive ventilation
Dr Kantroo mentions the following benefits of invasive ventilation:
- Gives requisite time window to heal the tissues
- Takes away load from respiratory muscles for them to heal
- Gives heart the benefit of offloading when it or any other organ is affected due to some disease.
“Day in and day out we see patients with a good baseline function and no major comorbidities who have benefitted out of invasive ventilation,” she says. “The duration of being on invasive ventilation differs from person to person; it can range from two to six weeks, although we have also seen people recover within 48 hours.”
Dr Padegal says that the majority of people come off the ventilator given that utmost care is provided.
Recovery
Dr Kantroo stresses the importance of physiotherapy and optimisation of medicines for recovery after getting off a ventilator. “The body must be kept active by moving the muscles regularly wherein blood circulation should be kept at a higher level,” she says. “It involves a holistic type of care which includes good nutrition by providing certain vitamins and high protein content.”