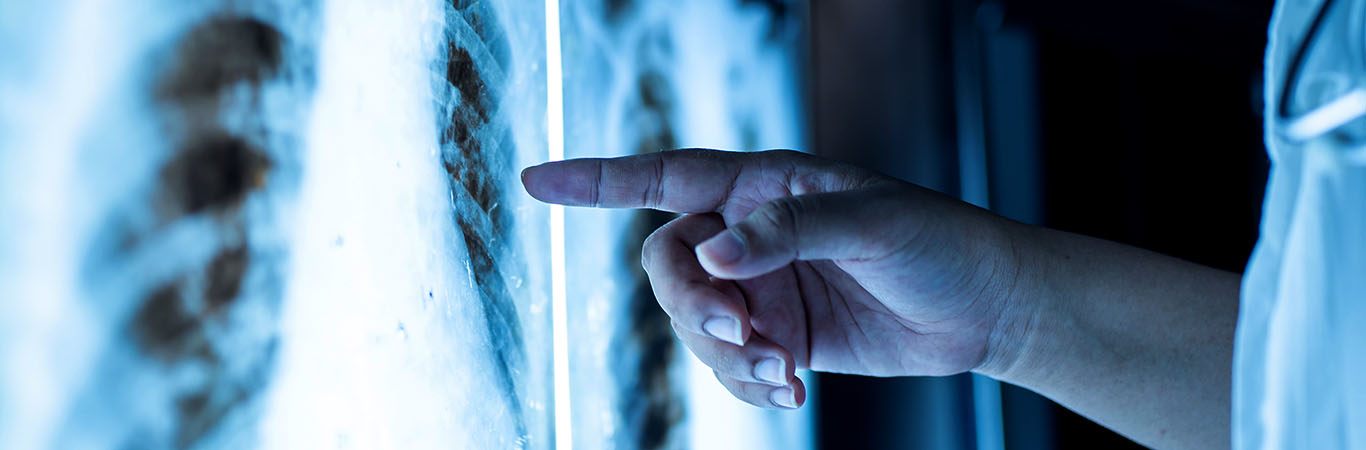
Bronchopneumonia is a type of pneumonia that infects and inflames the lungs. When children and elderly suffer from prolonged fever, cough and breathing difficulties, it can be a lung infection, known as bronchopneumonia.
In bronchopneumonia, the bronchus (the airway that connects windpipe to the lungs) is infected and inflamed. “The lungs have air sacs that get infected and filled with pus. They are scattered around the lungs and resemble multiple tiny pouches,” explains Dr Athul Francis, consultant pulmonologist, MAJ hospital, Edapally, Ernakulam, Kerala.
The condition can range from mild to severe.
Dr Nimish Shah, consultant pulmonologist, Jaslok Hospital & Research centre, Mumbai advises, one must immediately consult a doctor if fever, cough and phlegm is accompanied by sputum (mixture of saliva and mucus) and breathing difficulties. “When oxygen levels in the body dips alarmingly and breathing becomes difficult, it is a severe case of bronchopneumonia that may require hospitalisation,” adds Dr Shah.
Bronchopneumonia vs Lobar pneumonia
Bronchopneumonia affects people with weak immunity, those with comorbidities like obesity, diabetes, organ transplant recipients and those suffering from diseases like lupus or rheumatoid arthritis, says Dr Shah. Early diagnosis is crucial. It not only reduces the severity of the attack, it can also prevent the progression into lobar pneumonia, opines Dr Francis.

Dr Francis explains that the right and left lung are divided into sections known as lobes and the lobes further consist of smaller sections namely lobules. “What differentiates bronchopneumonia from other types of pneumonia is the density and pattern of spread in the infection. A typical chest X-ray for bronchopneumonia shows the pathogens within the lobules and they resemble multiple tiny, inflamed patches. When this is left untreated, this condition advances into lobar pneumonia where the entire lobe is infected causing denser inflammation and infections,” explains Dr Francis.
Bronchopneumonia: Who is at risk
“Those with weak immune systems like children below 5 years and elderly above 65 years are at risk. They can develop the infection in a shorter time compared to those with strong immune systems,” explains Dr Sachin Kumar, pulmonologist and critical care expert, Sakra World Hospital, Bengaluru.
Dr Kumar recalls the case of a 64-year-old man who had difficulty breathing, constant cough and fever in November 2022. His oxygen saturation levels (SPO2), on a pulse oximeter were critically low (84%), compared to the normal SPO2 between 95%-100%, says Dr Kumar. He had high blood sugar levels (300 milligrams per deciliter) and low blood pressure (90/60 mm/hg). A chest X-ray revealed multiple inflamed patches around the bronchus. It was bronchopneumonia.
Dr Kumar enumerates the other risk factors:
- Comorbidities such as allergies, chronic respiratory issues (COPD, asthma, bronchitis) or cardiac issues such as high blood sugar
- Aspiration pneumonia (where a part of food or liquid enters the lungs through windpipe instead of food pipe) or influenza
- Parkinson’s disease
- HIV, cancer, chronic kidney or liver disease and other immunocompromised conditions
- Long-term steroid use for medical conditions
- Environmental reasons such as smoking, constant exposure to irritants or chemicals from industries, living in crowded or unhygienic places
Causes of bronchopneumonia
Though viruses and fungi cause bronchopneumonia, over 80% of the infections for bronchopneumonia are bacterial, says Dr Francis. The most common bacteria are:
- Staphylococcus aureus
- Streptococcus pneumoniae
- Klebsiella pneumoniae
- Escherichia coli
Diagnosis
The first line of treatment is assessing breathing rate to understand the oxygen levels and oxygen saturation levels, says Dr Kumar. Further, Dr Shah enumerates the other tests:
- Chest X-ray – The easiest and reliable method for diagnosing the severity
- Complete Blood Count (CBC) – A blood test that helps assess the White Blood Cell (WBC) count in the body.
- C-reactive protein (CRP) test – A test that checks if the C-reactive protein in the liver is high.
- Procalcitonin (PCT) serum test – High PCT serum levels indicate bacterial infection in the lungs.
- Sputum culture – A test to identify the specific fungi or bacteria that is infecting the air passage.
Treatment for bronchopneumonia
The treatment includes intake of antibiotics, antifungal or antiviral medicines depending on the type of pathogen. Most mild cases of bacterial infections are cured within five to seven days. Severe cases require two to four weeks of antibiotics. Generally, in these cases the oxygen levels are low and the individual requires hospitalisation. Dr Kumar recalls the old man’s case. He was hospitalised, administered antibiotics and medications for BP and blood sugar while his diet was monitored.
Wholesome diet, rest and hydration plays a key role in recovery, say experts.
Prevention
Experts recommend vaccination (flu shots and pneumococcal vaccine) to prevent bronchopneumonia. Flu vaccines must be taken by everyone over six months of age, says Centers for Disease Control and Prevention(CDC). Pneumococcal vaccine is a must for:
- Those below five years of age
- Those above 60 years of age
- Those with comorbidities (diabetes, asthma, obesity)
CDC recommends pneumococcal vaccines to prevent infections caused by Streptococcus pneumoniae bacteria.
Wearing masks, gloves and exercising caution when spitting the mucus helps prevent the spread of the infection, says Dr Kumar.
Takeaways
- Bronchopneumonia infects the main airway in the respiratory tract.
- Children below 5 years and elderly above 65 years must exercise caution.
- Flu shots and pneumococcal vaccines can prevent infections.
- Wholesome diet, rest and hydration helps in recovery.