Researchers at the University of Southern California have developed a device to replicate a key feature of heart attacks in the lab.
This could allow us a better look at changes that take place in the heart after a myocardial infarction and even lead to the development of new heart drugs.
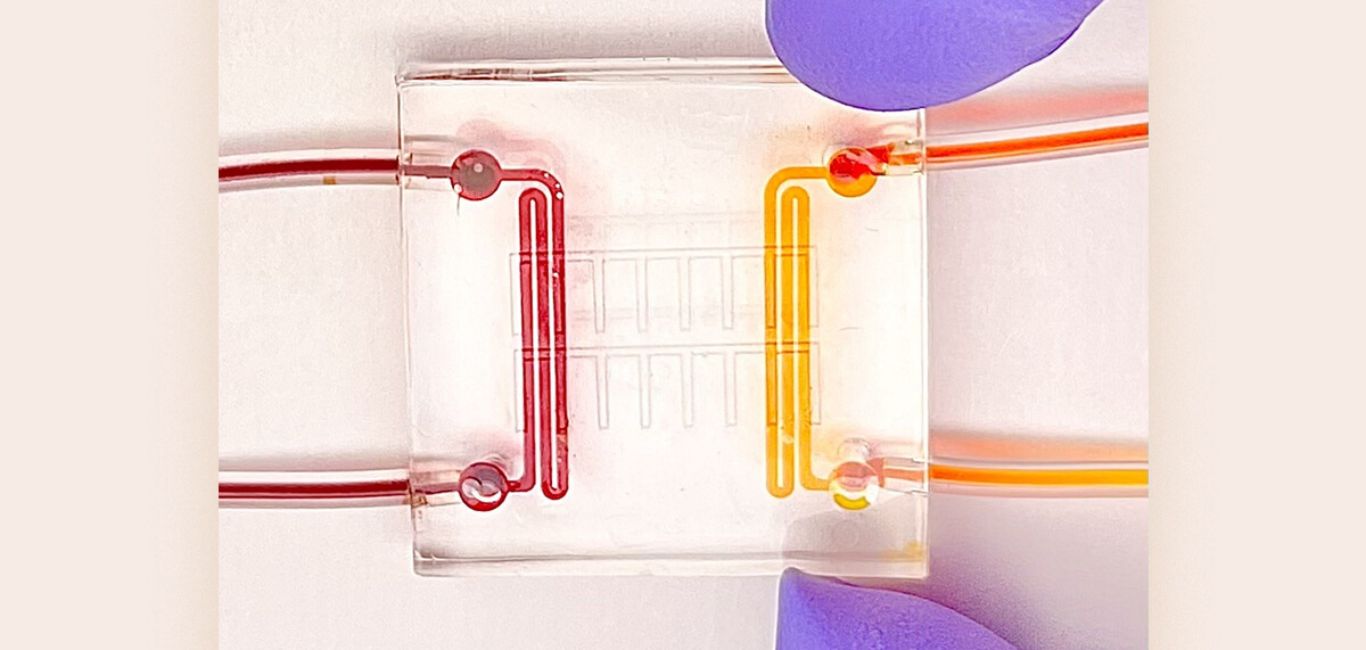
Dubbed a `heart attack on a chip’, the square microfluidic device which is 22 mm X 22 mm in size can simulate regions of heart cells that receive an abundance of oxygen and those that do not. What the researchers really aim to study is the border zone between healthy heart cells and dead or damaged heart cells.
The border region is an important region which can be salvaged with timely intervention.
“After a heart attack, the adjoining region between the injured, hypoxic tissue and the adjacent viable normal tissue — [which is also] known as the border zone — is characterised by an oxygen gradient [or difference],” the researchers wrote.
It is this border zone that we do not fully understand, especially changes in physical and chemical properties after a heart attack. Experts say this is also holding back the development of new type of therapeutics that can reverse or arrest the damage caused after a heart attack.
The heart-attack-on-a-chip model, which was demonstrated on rodent hearts, can aid in this. This is because researchers would be able to observe in real time certain functional changes in the heart – including arrythmia or an irregular heartbeat, and contractile dysfunction or decrease in the contraction strength of the heart.
“Our device replicates some key features of a heart attack in a relatively simple and easy to use system,” Megan McCain, PhD, an associate professor of biomedical engineering, stem cell biology and regenerative medicine at the USC Viterbi School of Engineering, said in a statement.
“This enables us to more clearly understand how the heart is changing after a heart attack. From there, we and others can develop and test drugs that will be most effective for limiting the further degradation of heart tissue that can occur after a heart attack,” she added.
Why heart attacks happen
A myocardial infarction (also known as heart attack) is commonly seen because of the formation of plaques in arteries. Plaques block the flow of blood in the arteries and thereby oxygen to heart tissues — which results in a cascade of events that lead to cell death.
The border region between healthy and dead heart cells also plays a role in pathogenesis (namely, the way any health disorder develops) and a lot of complications seen during an ongoing heart attack.
Validating the heart attack on a chip
To validate that the device was functional, the researchers at USC artificially induced a heart attack in the microfluidic device and studied the oxygen gradient in the engineered cardiac tissues. They also did RNA sequencing to study the expression of different genes during conditions of oxygen depletion.
“Engineered tissues, when exposed to different oxygen concentrations, showed border zone formations under hypoxia conditions and these border zones resulted in irregular calcium transport and inflammatory responses thus resulting in tissue damage and cell death,” according to McCain who was a corresponding author of the study.
These inflammatory responses were not observed in healthy tissues, which supported the role of oxygen depletion in tissue damage during heart attack. It was also observed that this oxygen depletion affected muscle contractions of the heart.
Gene expression studies further revealed that a particular gene called EREG was one of the top 5 five genes overexpressed during hypoxia conditions.
Role of microfluidics
The researchers said their study can aid in inventing a device for early detection of heart attacks, but it also allows testing of drugs that can effectively limit degradation of the heart tissue after a heart attack.
The in vitro model may also pave the way for developing and screening potential drug candidates for myocardial infarction in preclinical stages. It could also lead to the development of personalised medicines for individuals who have suffered heart attacks.
The researchers said that in the future, they may expand the uses of the model – for example, by adding immune cells or fibroblasts which generate the scar or repairing tissue after a heart attack.