Myocardial infarction, or a heart attack, is the leading cause of sudden adult deaths globally. When the heart’s lifeline of blood is disrupted, cells end up deprived of oxygen, leading to inflammation and fibrosis. In dire cases, traditional cures—drugs, angioplasty, bypass surgery—can falter.
The initial odds of survival in this heart-wrenching battle fluctuate, from one in ten with hospital care to one in three without it. This relentless killer is what drove Korean researchers to unearth a novel strategy of managing heart attacks — modulating the body’s own immune response.
Researchers from the Korean Institute of Science and Technology (KIST) and the Catholic University of Korea College of Medicine have tested an experimental therapy that promotes healing at the exact areas of the heart undergoing damage from a heart attack.
Also Read: Why the golden hour is crucial in heart attack response
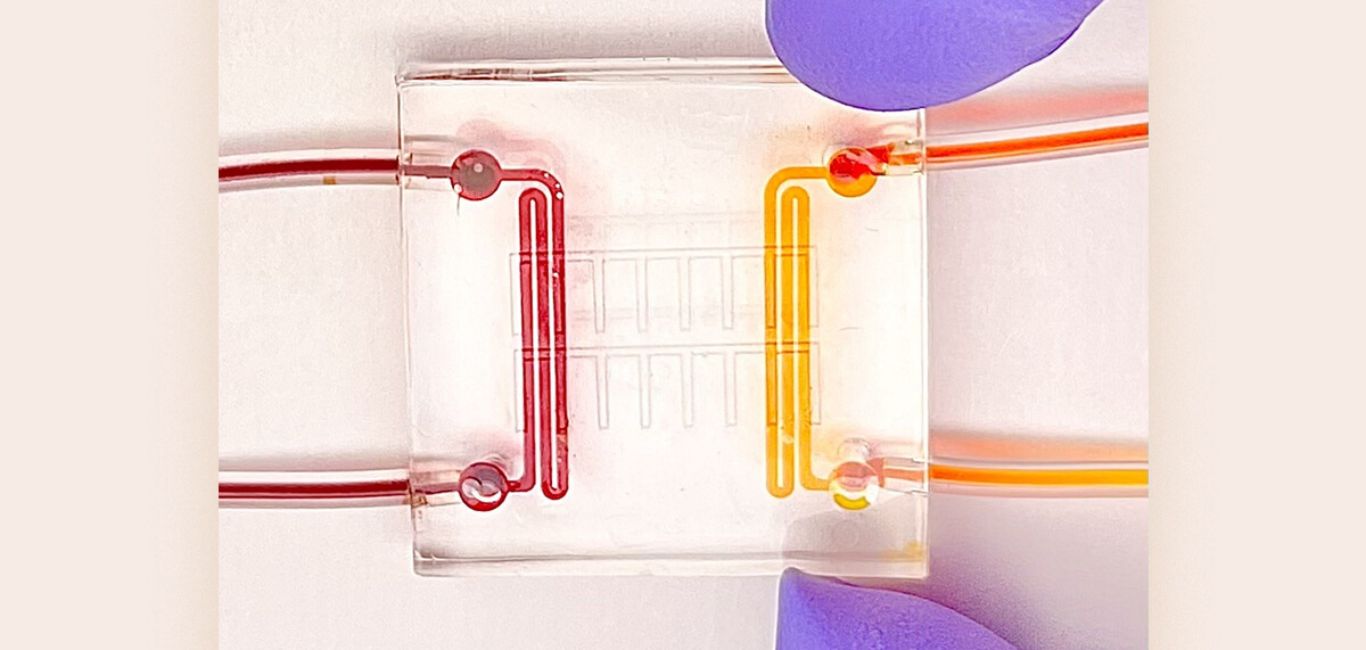
To achieve this, they utilized nanovesicles (small bubble-like structures) generated from apoptotic cells (cells with programmed self-destruction). They then adapted these bubble-like structures with specific proteins and substances to attract immune cells known as macrophages.
This adaptation enabled them to develop a medication that could precisely target the heart and decrease inflammation following a heart attack.
During mouse trials, they intravenously administered nanovesicles, effectively delivering them to macrophages at the myocardial infarction site. This resulted in reduced inflammation and enhanced heart function. They published these findings in the journal Advanced Functional Materials.
Also read: From stem cells to secretomes: The promise of more targeted therapies
“This is the first study to use nanovesicles produced from apoptosis-induced cells to treat myocardial infarction, and it has the advantage of being able to mass-produce them because it uses other cells rather than stem cells,” said Dr Yoon Ki Joung of KIST in a release.
“In the future, we plan to conduct research to verify the effectiveness and safety of the treatment, including clinical trials, through collaborative research with Catholic University of Korea Medical School and bio companies,” he added.
Preventative and personalised care
Speaking with Happiest Health, Dr Joung explains that the approach aimed to develop a preventative healthcare therapy for high-risk individuals. He stated, “If we apply our invented therapies to the clinic and advance them further, it reduces inconvenience and pain, and can even save the lives of patients suffering from the disease.”
However, this implies that the therapy cannot make itself available for emergency treatments. Dr. Joung states that to achieve the best treatment and effect, healthcare professionals must prepare the cell-derived nanovesicles in advance and administer them in a hospital.
Current research has also made use of nanovesicles derived from stem-cells to treat myocardial infarctions by modulating inflammatory response. The drawback, however, is that stem cells are difficult to produce in large quantities, limiting their economic viability.
Dr Young says their use of apoptotic cells in this therapy is a first, with many benefits. “Apoptotic cells can be easily prepared as compared to other cell types such as stem cells, engineered cells, or embryonic cells. It is cost-effective because we used commonly used adult cell line, fibroblast in the study.”
Another benefit of this approach is that it allows for personalised care, thanks to the autograft cells isolated from the individual who suffered a heart attack. “It is genetically and immunogenically safe because the used cell is dead cell,” he adds.
Significantly, Dr Joung says that the developed therapy can extend to most human conditions because it targets immune cardiology.
“[Since] many diseases are closely related to immunology and immune reactions, the invented therapy can be expended to most of human diseases, such as cancer, infectious diseases, and other immune-related diseases,” he says.
The therapy can also reduce the cost of healthcare, he adds.
KIST’s research accompanies many other advances in treating heart attacks. Dr Joung believes a combination of therapies for personalised treatment will be the right way forward. “Our invented technology will provide a novel and very strong option for the combination with existing treatments,” he says.