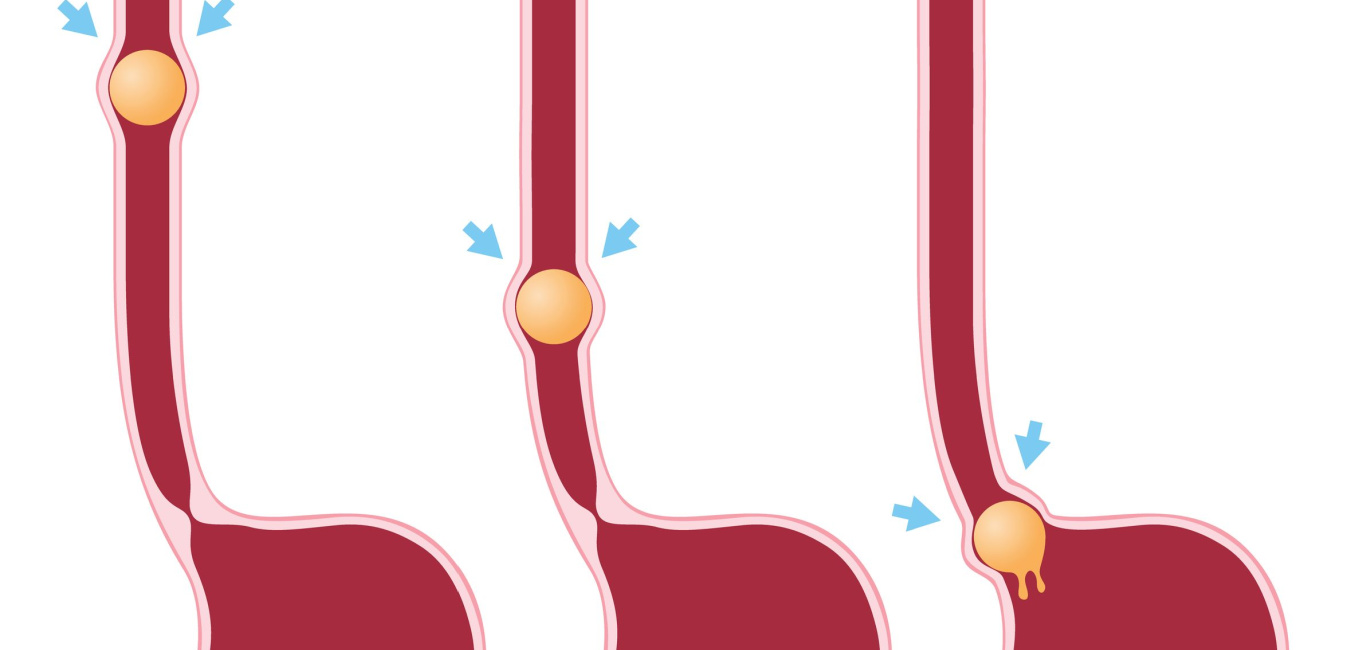
From that first juicy bite to the last drop absorbed, the winding path of digestion relies on the synchronised harmony of muscles and movements that steer food through the gut. “This rhythmic, wave-like contraction of smooth muscles in our digestive system is called peristalsis,” says Dr Harsh Shah, gastroenterologist and hepato-biliary pancreatic surgeon, Apollo Hospital, Ahmedabad.
Peristalsis keeps things moving smoothly, so food spends the right amount of time in each part. This allows proper digestion and nutrient absorption. Even the rumbling when you’re hungry results from peristalsis contractions. When this intricate process gets out of sync, disruptions from constipation to vomiting can occur, underscoring the importance of healthy peristalsis for orderly digestion.
It begins when you swallow, as muscles squeeze the food down the oesophagus into the stomach. In the stomach, peristalsis churns food into a liquid mixture. It continues as food moves through the small and large intestines, until nutrients are absorbed and waste is removed, explains Dr Shah.
Stretch receptors play important role in peristalsis generation
Lining the digestive tract are stretch receptors that detect food passing by. This stretching sensation triggers the nervous system to initiate muscle contractions, says Dr Shah.
Propagation of peristalsis wave is a complex process which requires intricate interplay of nerve, muscles, and electric signals. Specialised cells that act like pacemakers (called interstitial cells of Cajal) generate electric signals that make the muscles contract as a wave down the digestive highway.
These slow waves pass on to the surrounding smooth muscle cells and contract them. This contraction wave goes on progressively down the gastrointestinal tract, he explains. Generation of the peristalsis can occur even in the absence of stimulus such as food.
When it goes wrong
Understanding peristalsis matters because when this intricate sequence of muscle contractions goes awry, it can trigger digestive issues or even systemic health problems. For instance, impaired peristalsis can cause constipation from slowed movement, diarrhoea from poor absorption, and vomiting from delayed stomach emptying.
Identifying and treating the underlying peristaltic dysfunction is key to preventing such complications and maintaining overall wellbeing. After all, the gut’s muscular motility influences far more than just digestion – it is intrinsically tied to our nutrition, immunity and metabolism.
Health issues that can be caused by impaired peristalsis
When peristalsis is impaired, various health issues can arise. Dr Shah breaks down these conditions below:
- Constipation: Slow peristalsis in the large intestine leads to hard and dry stools which are difficult to pass.
- Diarrhoea: Impaired peristalsis hinders food absorption in the small intestine, leading to diarrhoea due to malabsorption, infection and increased gut motility.
- Gastroparesis: Occurs when the stomach gets weakened and paralysed due to impaired peristalsis leading to delayed emptying, nausea, vomiting, bloating, and early satiety.
- GERD (Gastroesophageal Reflux Disease): Impaired lower oesophageal sphincter (LES) causes stomach contents to move back to the oesophagus. Symptoms include acidity and heartburn triggered by acid reflux, and chest pain.
- Achalasia cardia: Occurs when the LES does not relax properly, making the entry of food into the stomach difficult and leading to difficulty swallowing. Food may get stuck in the chest, causing regurgitation and chest pain.
- Intestinal pseudo-obstruction: In this condition, though there is no mechanical blockage, peristalsis is absent, resulting in food not moving at all to the large intestine. It can be caused by post-abdominal surgery, infection, and/or electrolyte disturbances.
Management of peristaltic disorders
Management of peristaltic disorders depends upon identification of the underlying cause and different health conditions resulting out of it. For example, people having constipation are given laxatives or bulk laxatives which are fibres, explains Dr Shah.
“If the person is having diarrhoea due to infection, it should be treated with antibiotics. If it is non-infectious then medications are given to reduce the peristaltic frequency. The modulation of gut microbiota can also be done by probiotics which also relieves underlying symptoms,” says Dr Shah.
There are certain medicines which increase the stomach peristalsis activity and can be used for gastroparesis. In achalasia cardia, surgical intervention is done to loosen the lower oesophageal sphincter which has become tight, Dr Shah elaborates.
Tips to maintain healthy peristalsis
Besides the conditions requiring the surgery, those with impaired peristalsis can be helped with the following lifestyle modifications.
- Increase fibre intake with fruits, vegetables, whole grains, beans, and legumes.
- Staying hydrated by drinking at least 8-10 glasses of water daily to soften stools
- Regular physical activity or exercising of at least 30 minutes daily – walking, swimming, cycling or any exercise of choice. Avoid prolonged sitting; try to take a break once every hour to stretch and move.
- Management of stress is useful as it can also affect gut microbiota and peristalsis. People are advised to practise relaxation techniques by means of yoga, meditation, and deep breathing exercises.
- Get 7-8 hours of sleep. Sleep deprivation can negatively affect peristalsis and digestion.
“Along with these, one should be mindful of what they eat. Overeating or staying hungry for longer duration of time should be avoided. Food should be chewed properly, as digestion and peristalsis get affected by improper chewing of food particles. All these measures will help a person in maintaining health peristalsis,” advises Dr Shah.