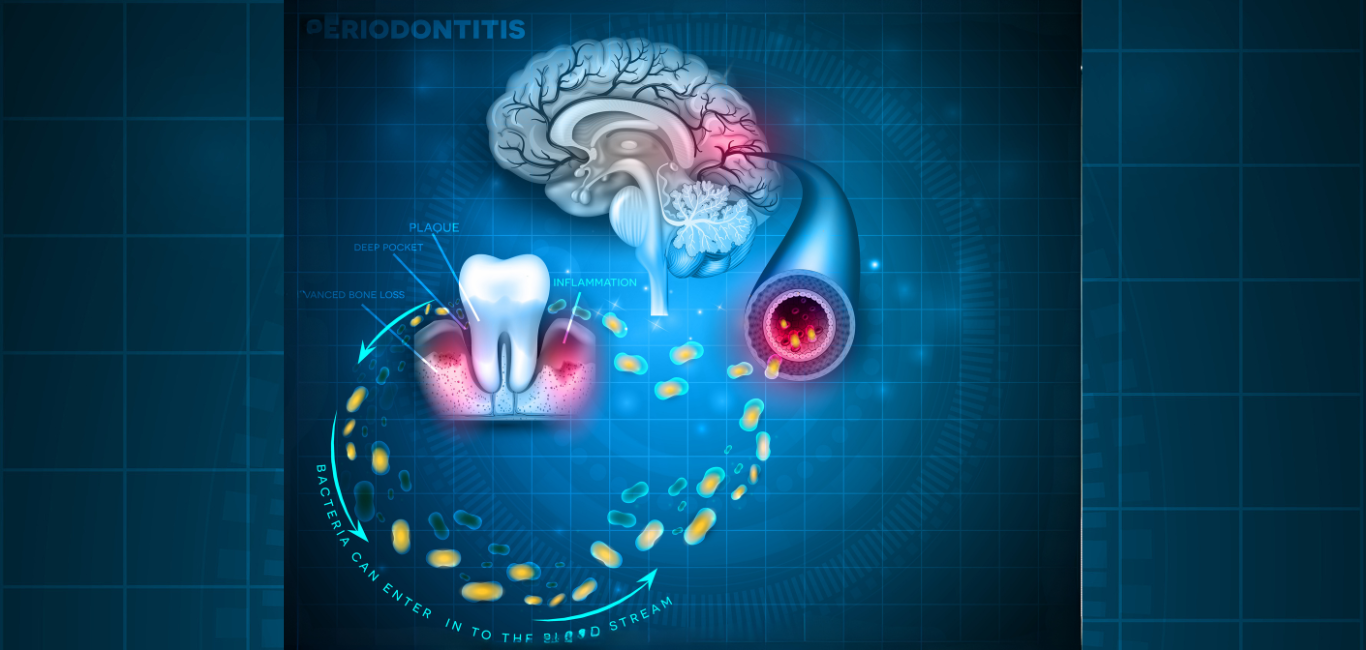
We are all aware of the importance of maintaining our oral health, and for good reason. Lack of proper oral hygiene can lead to harmful bacteria accumulating in the mouth, resulting in: bleeding gums, loosening of teeth, bad breath, cavities and tooth sensitivity.
Studies have even shown that these problems are not just confined to the mouth; they can affect the colon, the heart and the brain. Yet, the exact mechanism of how oral bacteria affects the brain had not been fully understood.
Researchers from the Forsyth Institute, Massachusetts, aimed to bridge that gap. Their study—published in the Journal of Neuroinflammation—made a breakthrough in understanding how oral bacteria could potentially be linked to developing Alzheimer’s.
“In this study, we were asking the question, can oral bacteria cause a change in the brain cells,” says Dr Alpdogan Kantarci, senior author of the study, in a statement.
Amyloid beta and tau proteins are by-products produced in the brain when neurons communicate to transfer signals (forming synapses). Special immune cells called microglia remove these excess proteins to keep the brain healthy. However, in Alzheimer’s, the amyloid beta and tau proteins accumulate, choking the nerve cells and causing neurodegenerative conditions.
In their experiments, the researchers observed that poor oral health resulted in excess deposits of these toxic proteins. They assessed gum disease progression and oral bacteria growth in mice. Simultaneously, they used molecular techniques to assess the rats’ brain cells.
Researchers introduced oral bacteria in the gums of the mice and observed the growth of bacteria for four weeks. After 30-days, the researchers found that an oral bacteria called Klebsiella variicola had entered the mice’s brains. That was not all. These bacteria were affecting the microglia, making them overactive and causing neuron inflammation.
To cross-check the bacteria’s effects, the researchers took microglia cells from healthy mice and grew them in the laboratory. Then, they exposed these colonies of healthy microglial cells to Klebsiella variicola.
Read more: How do gut bacteria ‘taunt’ Alzheimer’s
Read more: Bleeding gums: dentists’ guide to restoring healthy gums
They noticed a similar effect: the bacteria altered the microglial cell activity and caused the overstimulation of these cells. The over-activity of microglia affected their ability to break down amyloid-beta plaques. “They [microglia] basically became obese and no longer could digest plaque formations.” Dr Kantarci said.
“The interaction of microglia with oral bacteria significantly alters the functions of microglia cells by increasing the neuroinflammation process and phagocytosis of the toxic proteins, amyloid beta,” the study’s authors say.
Dr Shabeer Ahamed, periodontist and professor from Malabar Dental College and Research Centre, Malappuram, Kerala, agrees. He says that bacterial infection in the oral cavity and chronic inflammation because of gum disease could cause brain degeneration. “Microorganisms [living in the oral cavity] arising from the localised infection [gum disease] spread the infection to other parts of the body, resulting in a chronic and systemic condition [neurodegenerative conditions],” he says.
Another study published in July this year by researchers from Tohoku University in Sendai, Japan, revealed that oral disease shrinks the hippocampal brain area. This brain region is associated with memory formation, and its shrinkage leads to neurodegenerative conditions like Alzheimer’s. The findings indicate that teeth with severe gum disease are associated with brain shrinkage.
Emphasising proper oral hygiene, Dr Ahamed said that regular dental check-ups and cleaning of teeth every six months are required to maintain healthy gums.
Researchers of the current study also emphasise the need for controlling the oral inflammation associated with gum disease, as it can increase the risk of neurodegenerative conditions.