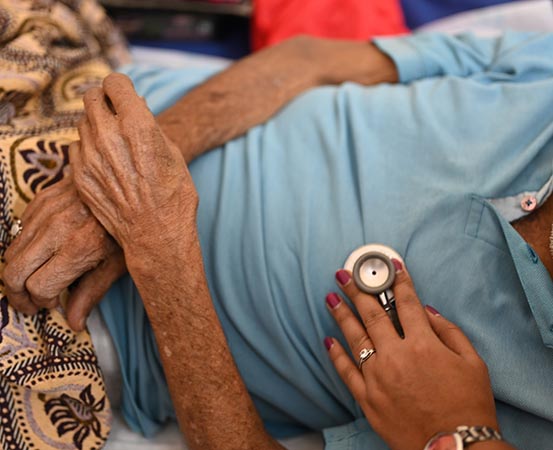
No improvement from a chronic illness and no relief from pain can be traumatic. When people no longer have a chance of complete recovery from a condition, it can cripple their quality of life. But palliative care can offer a helping hand.
Palliative care is a caregiving approach for those who no longer have a chance of complete recovery or the possibility to reverse the disease. Elderly persons who are suffering from chronic conditions like cancer, end-stage renal disease, cardiac disease and life-limiting neurological issues like stroke, Parkinson’s and dementia potentially come under the purview of palliation.
READ MORE :
How to patch up that abnormal gait
How to prevent bedsores in older people
Managing delirium among elderly people
Malnutrition: how to spot the signs in older people
Palliative care entails managing painful symptoms that either start slowly or quickly and worsen over time. “Treatment in the initial days involves painkillers like paracetamol tablets and morphine, where the dose is gradually increased depending on the severity of the pain,” says Dr Joydeep Ghosh, internal medicine specialist, Fortis Hospital, Kolkata.
Bubul Choudhury, 60, a businessman from Assam, wishes that he knew about palliative care when his mother’s cancer resurfaced three years ago. “When there was no scope for recovery, we tried our best to make her life as comfortable as possible,” says Choudhury, who got his mother palliative care when it became impossible to soothe her pain as her condition progressed.
Although his mother passed shortly after, he says that she was at peace as palliative care provided much-needed relief to her uncontrollable pain.
Palliative care focuses on improving a person’s quality of life by addressing the needs rather than the prognosis. “Palliative care is not meant to cure the disease; it is just giving them the supportive treatment which can give relief from the symptoms,” says Dr Ghosh.
Dr Raghavendra Ramanjulu, a palliative care specialist from Aster CMI, Bengaluru, says that palliation, which means to ‘fight over a crisis’, starts from the date of diagnosis of the chronic illness.
Who can opt for palliative care?
Dr Ramanjulu lists out certain symptoms among those suffering from chronic illnesses which decide whether the person needs palliative care therapy or not:
- Chronic pain
- Breathlessness
- Cough
- Nausea
- Vomiting
- Constipation
- Delirium
- Sweating
- Fatigue
According to Dr Ramanjulu, palliative care looks at the total pain concept where treatment covers all aspects of well-being: the physical, emotional, social and economic health of a person affected. “Treating through pain relief medication, addressing the issues of anxiety, depression, improving their quality of life, looking into the spiritual well-being is what we focus on,” he adds.
Emotional well-being is critical
The importance of emotional well-being is an integral part of palliative care which needs to be emphasised more, points out, Dr Ghosh. “Palliative care also involves making sure a person has support groups and counselling sessions with a psychiatrist to manage symptoms of anxiety and depression,” he explains.
He adds that psychological support is also extended to caregivers whose mental health takes a toll when a family member is diagnosed with a life-threatening illness. This can be in the form of counselling or psychotherapy.
Multi-speciality team
Listening to the person in palliative care is the thumb rule in this approach. “We ensure that not just the caregivers, but also the affected person has a say,” says Dr Ghosh.
Experts from different specialities work in tandem when it comes to palliative care and make decisions. “Palliative care involves a team of specialists, not just a single doctor,” says Dr Ramanjulu. He adds that there is a team involved, including a trained palliative medicine specialist, nurses and coordinators who make sure palliation is achieved smoothly. Besides, the team includes physiotherapy rehabilitation groups, occupational therapy groups for gait building, psychiatrists and psychologists.
Takeaway: palliative care is not the end of life
End-of-life care or hospice care is an extension of palliative care which aims at providing relief to those nearing the end. However, end-of-life care and palliative care are not the same, say doctors. “Palliative care helps improve not only the quality but also the dignity and longevity of life. So, palliation is not just about the end of life. In fact, it also improves the quality of life for the caregivers too,” says Dr Ramanjulu.

















