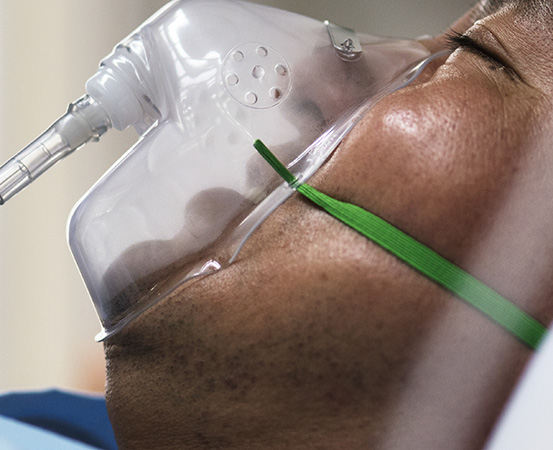
Big surprises come in small packages. Just about the size of lunch boxes, the non-invasive machines — CPAP (continuous positive airway pressure) and BiPAP (Bi-level positive airway pressure) — may just be the ‘go-to ventilators’ for those having breathing trouble. They are a form of respiratory therapy that pushes air into the airways with positive pressure and opens the lungs to facilitate seamless breathing. The therapy is non-invasive in which air is delivered through a special face mask with a tight seal.
This is different from conventional invasive procedure via tracheostomy which requires an incision in the windpipe to aid breathing.
Dr Nikhil Modi, a senior consultant at the department of respiratory critical care and sleep medicine, Apollo Hospital, Delhi, says these machines have changed the health outcome of many people. He recalls the case of a sixty-five-year-old man with advanced chronic obstructive pulmonary disease (COPD) who required admission to the hospital due to his ever-increasing breathlessness with cough and infection almost every month. He was advised to use non-invasive positive airway pressure at home and his need for hospitalisation decreased considerably.
READ MORE:
Warm and humidified air – the magic of nasal cannula
Mechanical ventilation: invasive but life-saving
Chest drain: letting your lungs breathe
Prone position ventilation, a lifesaver
Dr Vivek Anand Padegal a senior pulmonologist at Fortis Bengaluru says the use of non-invasive ventilators has significantly shortened hospital stays.
It has also reduced the dependency on invasive respiratory therapies, like in the case of Nagamma, a 50-year-old woman from Hyderabad who experienced breathlessness and was admitted to the emergency wing of a hospital after she tested positive for covid-19 in February 2021. She says the positive airway pressure ventilator saved her life.
Types of non-invasive positive airway pressure ventilators
There are two types of non-invasive ventilators with a primary difference in the kind of pressure they develop.
“Their usage depends on the specific health condition and need of a person,” says Dr Nikhil Paul, assistant professor of emergency medicine at Sree Gokulam Medical College, Kerala. The two types of machines are:
- CPAP — Continuous positive airway pressure
- BiPAP — Bilevel positive airway pressure
“CPAP and BiPAP ventilators can either be two different machines or a single machine with both the settings,” he says. “The single-setting machines are usually used at home while the ones in the hospital come with both settings,” adds Dr Paul.
“Most ICU patients need BiPAP when they are unable to breathe on their own, while CPAP is used sometimes in the ICU and mostly at home,” points out Dr Padegal.
Understanding the CPAP machine
Explaining the working of CPAP, Dr Paul says, the device delivers air with continuous pressure. That means the pressure during inhaling and exhaling remains the same. “This constant pressure aids oxygenation in people who are experiencing hypoxia (reduced oxygenation inside the lungs) by delivering enough oxygen to the lungs and facilitating sufficient oxygen exchange by opening the airways,” he says. He adds that people with obstructive sleep apnea (OSA), congestive heart failure, obesity and a thick neck experience hypoxia and benefit significantly from using the CPAP ventilator.
Dr Modi says that CPAP significantly reduces the effects of OSA and the risk of cardiac ailments.
It was CPAP ventilation that helped manage Nagamma’s breathlessness recalls her husband while speaking to Happiest Health.
The BiPAP machine
“The BiPAP ventilator as the name suggests, pushes air into and out of the lungs with two different levels of pressure,” says Dr Paul. “The inspiratory (inhaling) pressure is more than the expiratory (exhaling) pressure.”
Explaining the reason for two different levels of pressure, Dr Paul says that BiPAP makes breathing out easier for people with COPD who expend a lot of energy breathing.
Can people switch from CPAP to BiPAP if they find continuous pressure very uncomfortable?
The national sleep foundation (NSF), a US-based government agency says that sleep specialists or doctors are unlikely to place a person on BiPAP unless they cannot tolerate CPAP at all.
The CPAP, BiPAP complications
Dr Paul has observed that using a CPAP or BiPAP ventilator is not a very pleasant experience for people especially since the usage is long-term. He says that it is challenging for people because of the claustrophobia the machine could cause; the huge airtight mask not only covers the mouth but also most of the face.
Speaking on the other medical implications of the ventilators, Dr Paul says that sometimes too much positive pressure can cause a condition called pneumothorax which occurs when air leaks into the space between the lungs and chest wall. The additional pressure can also cause air to enter the stomach, causing abdominal distension, leading to gastritis, nausea and vomiting.
“Infections are rare as oxygen is in a dry form, but they can occur if the mask is not cleaned properly with warm water after every use,” he warns.
Dr Padegal says occasionally the machines can cause pressure ulcers (injuries to the skin because of prolonged pressure) due to oxygen being pushed onto the face with continuous pressure.
Nagamma developed itchy skin on her face. “She kept complaining of a burning sensation, especially around her mouth, and would get so uncomfortable that she would try to throw away the mask sometimes,” says her husband.
The brighter side
“Although most people get accustomed to the initial discomfort of using the ventilator, the ones who don’t are given sedatives to help relax and facilitate bronchodilation (opening up of the airways),” says Dr Paul.
A case study published in the BMJ journal talks about a possible solution for ventilator intolerance. The study reveals how a combination of different surgical methods helped a 55-year-old BiPAP-intolerant person dealing with OSA increase his compliance levels with the machine.
The ventilators come with automated settings and can be easily used at home without the help of a nurse, or a professional caretaker says Dr Paul who adds that another significant advantage of using non-invasive positive airway pressure ventilation is that people never get addicted to this therapy.
Some people have reduced their dependency on these machines and use them sparingly.
A septuagenarian (name withheld for privacy) from Nagpur dealing with COPD shares with Happiest Health how pranayama helped him immensely. He says that within just six months of practising pranayama, he was able to strengthen the capacity of his lungs and gradually reduce his dependency on the CPAP machine.
But Dr Paul also says a person using the machine cannot be left unattended. “If the machine malfunctions, the person can develop breathing difficulties and further complications,” he explains.
Adaptive servo-ventilation (ASV)
ASV is a type of non-invasive ventilation. It is a more specialised machine that measures the breathing patterns and customises the pressure delivered to stabilise breathing throughout the night. It is generally used to manage central sleep apnea (CSA), a problem where one does not take enough breaths in a minute — the breathing rate is either too slow or there are long pauses without breathing.

















